The Mechanism of Action of Diuretics

Source: http://www.bbc.co.uk/health/healthy_living/complementary_medicine/remedies_supplements.shtml
Diuretics are drugs that increase the output of urine. There are four main classes of diuretics (b through e, below). In addition, functions of each portion of the nephron will be discussed (a), as well as conditions for which diuretics are prescribed (f)
Functions of Each Portion of the Nephron (Soleil)
The human body has two kidneys that function mostly to clear wastes from the blood and secrete them along with urine. However, the kidneys also regulate pH, blood pressure, and plasma volume as well as secrete hormones. Within the kidney there are units called nephrons that start with a glomerulus and continue with the proximal convoluted tubule, loop of Henle – descending and ascending limb, distal convoluted tubule, then finally to the collecting duct and out of the kidney to the ureters, bladder, urethra, then out of the body. There are over one million nephrons per adult kidney.
Below is a cartoon/pictorial of the nephron taken from RFUMS lectures by Dr. Darryl Peterson:

Filtration of blood and formation of the urine starts in the glomerulus which is a capillary bed surrounded by Bowman’s capsule and located in the cortex, or outer portion of the kidney. Blood flows into the capillary bed through the afferent arteriole and filters through the filtration barrier which consists of endothelial cells of the glomerular capillaries, the basal lamina or basement membrane, and podocytes of the visceral layer then blood flows out of the capillary bed through the efferent arteriole. Glomerular ultrafiltrate, which includes ions (Na+, K+, Ca2+, PO4), metabolic waste products (urea, creatinine, organic acids), glucose, amino acids, and water is filtered into the proximal convoluted tubule. Filtration pressure (usually 24 mm Hg) is the net pressure from capillary hydrostatic pressure (roughly 60 mm Hg), oncotic pressure (roughly 21 mm Hg), and capsular hydrostatic pressure (roughly 15 mm Hg) giving the equation: 60 – (15+21) (RFUMS). This drives ultrafiltrate through the filtration barrier and into the next portion of the nephron called the proximal convoluted tubule (PCT).

Above is a slide found from virtual microsope of a glomerulus and Bowman's capsule. Note the start of the proximal convoluted tubule at the urinary pole in the lower portion. Also note the vascular pole with afferent and efferent arterioles on the opposite pole.
The PCT is an important site for resorption hence the brush border with microvilli which increases surface area for resorption. Here is where 2/3 or 67% of filtered Na+ and H2O are reabsorbed (Costanzo). Reabsorption of Na+ and H2O is isosmotic therefore exactly proportional. Na+ is reabsorbed in the early proximal tubule via cotransport with glucose, amino acids, phosphate, and lactate or via countertransport with a Na+-H+ exchange linked directly to reabsorbed HCO3-. All glucose and amino acids, 85% of phosphate (the other 15% is excreted in the urine), and most lactate are reabsorbed here (Costanzo). In the middle and late proximal tubules Na+ is reabsorbed with Cl-. The PCT also reabsorbs 50% of filtered urea, 67% of filtered K+ along with Na+ and H2O, filtered Ca2+ by passive processes coupled to Na+ reabsorption, and Mg2+ (Costanzo). Ammonia is also secreted here to act as a buffer for secreted H+.

Above is a slide found on virtual microscope of proximal convoluted tubules. Note the brush border in the lumen. Also note basal striations. In the lower left, a tubule with a clear lumen is visible; this is the distal tubule.
The filtrate moves from the PCT to the thin descending loop of Henle which is impermeable to salts but does passively reabsorb water due to the gradient that is set up in the interstitium of the medulla. As the filtrate descends down the loop deeper into the medulla, the interstitium is more hypertonic and water flows out of the lumen and is reabsorbed. These limb lengths are dependent upon where the nephron is located in the kidney. Cortical nephrons will have thick descending limbs and shorter thin descending limbs as opposed to juxtamedullary nephrons that have longer thin descending limbs. The longer the limb, the more concentrated the urine will become because the more time the interstitium has to reabsorb water.
Filtrate then moves onto the thick ascending limb which actively reabsorbs Cl-, 25% of filtered Na+, and 20% of filtered K+ using the Na+-K+-2Cl- cotransporter (Costanzo). This indirectly helps reabsorption of Mg2+ and Ca2+. This portion of the nephron is impermeable to H2O. The hormone aldosterone can also stimulate Na+ and Cl- reabsorption here.

Above is a slide found from virtual microscope of the ascending and descending limps of the loop of Henle. Note the descending limbs with the brush border and the ascending limbs with the clearer lumen.
The filtrate then moves to the distal tubule where 8% of filtered Na+ is reabsorbed using a Na+-Cl- cotransporter and K+ is reabsorbed if there is low dietary intake of K+ (Costanzo). Parathyroid hormone controls the reabsorption of Ca2+ here. This section is also impermeable to H2O. The juxtaglomerular complex is a special region of the distal convoluted tubule which is located close to the afferent and efferent arterioles of the renal corpuscle. It reacts to the hormone Renin and helps regulate fluid volume, blood pressure, salt and water.

Above is a slide from virtual microscope of the juxtaglomerular complex. Note the clearly visible Macula Densa cells of the distal tubule on the right side.
In the late distal tubule and the collecting duct principal cells reabsorb Na+ and H2O and secrete K+. These cells can react to antidiuretic hormone which helps increase water permeability by adding aquaporins onto the apical plasma membrane therefore urine is more concentrated. These cells can also react to aldosterone which will increase Na+ reabsorption and K+ secretion. The other type of cells here are α-intercalated cells which reabsorb K+ using an H+-K+ ATPase and in response to aldosterone secrete H+. Antidiuretic hormone also increases the urea permeability in the collecting duct. The late distal tubule and collecting duct actively reabsorbs 8% of filtered Ca2+. The distal tubule also reabsorbs Mg2+ (Costanzo).

Above is a slide from virtual microscope of the collecting ducts. This slide is from the papillary region because note the connective tissue between ducts.
From here the filtrate moves on to the ureters then the bladder and out of the body as urine via the urethra.
Each diuretic targets specific segments in the nephron. Below is a useful picture to keep in mind as each type of diuretic is discussed.

Source: http://sprojects.mmi.mcgill.ca/nephrology/presentation/presentation3.htm
Osmotic Diuretics (Sinh)
- Normal Molecular Mechanism of the Transporter Affected by Osmotic Diuretics:
Normally, 65-80% of the filtered water, sodium, and chloride is reabsorbed in the proximal tubule. Additionally, most bicarbonate and all of the glucose are reabsorbed here also. Water is permeable in both the proximal convoluted tubule portion and the thin descending limb.
The regular mechanism for water transport in the proximal tubule can be summarized as follows. Na-K-ATPase transports Na+ from the basement membrane of the renal epithelial cell to the intercellular and interstitial space. This reduces the concentration of Na+ inside the cell and creates an electrochemical gradient that allows Na+ from the filtrate in the lumen to diffuse into the cell at the apical surface. Taking advantage of the free-energy of the Na+ gradient, other solutes utilize various co-transporters to move into the cell from the lumen. As all this takes place, water follows the movement of the solutes via the osmotic gradient. Hence, water is pulled into the intercellular space from the cell, which pulls it from the tubule. The net effect is reabsorption of water and solutes in the proximal tubules and descending limb.

S, symporter; A, antiporter; CH, ion channel; WP, water pore; U, uniporter; ATPase, Na+,K+-ATPase (sodium pump); X and Y, transported solutes; P, membrane-permeable (reabsorbable) solutes; I, membrane-impermeable (nonreabsorbable) solutes; PD, potential difference across indicated membrane or cell.
Source: http://online.statref.com/Document/Document.aspx?DocId=264&FxId=75&Scroll=1&Index=0&SessionId=82BFF1LYFJTGYVXJ
- Mechanism of Action of Osmotic Diuretics:
Osmotic diuretics are solutes that help draw water back into the lumen by creating an opposing osmotic force. These osmotic solutes have limited reabsorption in the nephron; hence they are able to maintain the opposing osmotic force and keep water in the tubules. The decrease in water reabsorption also creates a back-flow of sodium back into the tubule.
Four currently available osmotic diuretics are glycerin (OSMOGLYN), isosorbide (ISMOTIC), mannitol (OSMITROL), and urea (UREAPHIL). (Source: Stat!Ref)

Source: http://online.statref.com/Document/Document.aspx?DocId=264&FxId=75&Scroll=1&Index=0&SessionId=82BFF1LYFJTGYVXJ
- Overall Effect of Osmotic Diuretics on Kidney Function:
The result is an increase in water and sodium excretion and urine production. Excretion of nearly all solutes, including Na+, K+, Ca2+, Mg2+, Cl-, HCO3-, and phosphate, are also increased. Osmotic diuretics act on the loop of Henle and the proximal tubule. In the body, osmotic diuretics extract fluid from intracellular components and increase extracellular fluid volume. As a result, blood viscosity is decreased, RBF is increased, and renin is inhibited in the kidney. The increased RBF occurs as a result of dilated afferent arterioles (increases PGC) and dilute plasma (decreases PGC). However, GFR shows little change because of the increase in PT.
A rapid decrease in GFR, i.e., acute renal failure (ARF), is a serious medical condition in many hospitalized patients. Although studies on animal models show that mannitol is effective in counteracting the decrease in GFR, the effect of mannitol on people is less established in scientific studies. Below is a comparison table of common diuretics.

Source: www.rcoa.ac.uk/docs/B8_Primary.pdf
Carbonic Anhydrase Inhibitors (Christine)
- Normal Molecular Mechanism of the Transporter Affected by Carbonic Anhydrase Inhibitors:
The regulation of bicarbonate levels is important for acid-base balance. The majority of bicarbonate that is filtered through the glomerulus is absorbed in the proximal tubule. This is equal to roughly 80%.
 Source: http://grove.ufl.edu/~weineid/RenalLectures/MS1/Acid-base.pdf
Source: http://grove.ufl.edu/~weineid/RenalLectures/MS1/Acid-base.pdf
Carbonic anhydrase (CA) is essential for bicarbonate reabsorption. Carbonic anhydrase can be found in two locations within the proximal tubule: 1) bound to the apical membrane, and 2) free within the cytosol. It functions to interconvert carbon dioxide (CO2) and water (H2O) to carbonic acid (H2CO3). Carbonic acid then readily dissociates to form a proton (H+) and bicarbonate ion (HCO3-). It performs the following reaction:
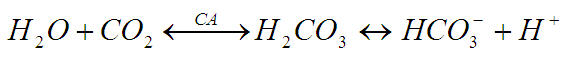
Since the filtered bicarbonate entering the proximal tubule is charged, it has difficulty crossing the lipid membrane of the tubular cell. In order to convert the charged ion to a non-polar form, which can enter the cell with greater ease, the filtrate must be acidified. Hydrogen secretion is accomplished by the H+/Na+ exchanger in the apical membrane of the renal tubular cell. This secondary active transport reaction is ultimately driven by a Na+/K+ pump in the basolateral membrane of the cell. The proton that is secreted into the lumen of the tubule readily associates with filtered bicarbonate to form carbonic acid. Carbonic anhydrase present in at the apical border of the cell converts the carbonic acid to form water and carbon dioxide. As a result, water and carbon dioxide can passively diffuse into the cell.
 Source: http://grove.ufl.edu/~weineid/RenalLectures/MS1/Acid-base.pdf
Source: http://grove.ufl.edu/~weineid/RenalLectures/MS1/Acid-base.pdf
Once in the cell, the water and carbon dioxide must be reconverted to bicarbonate ion in the opposite reaction as above by cytosolic carbonic anhydrase. The intracellular concentration of bicarbonate increases, driving the passive movement of bicarbonate down its electrochemical gradient and across the basolateral membrane. Sodium is transported with bicarbonate out of the cell via the Na+/HCO3- symporter and into the interstitium. The end result is sodium bicarbonate absorption into the blood.
- Mechanism of Action of Carbonic Anhydrase Inhibitors:
Carbonic anhydrase inhibitors are a class of diuretic that disrupt normal function of both the membrane-bound and cytosolic forms of carbonic anhydrase. The formation of carbon dioxide is reduced and bicarbonate cannot be reabsorbed from the filtrate. Consequently, sodium absorption is also reduced due to low intracellular hydrogen formation. Water passively follows sodium movement and thus remains within the kidney tubule and ultimately excreted.
Acetazolamide is an example of a carbonic anhydrase inhibitor. It is most often administered, not for its diuretic property, but as treatment for glaucoma, epilepsy, intracranial hypertension, and altitude sickness.
- Overall Effect of Carbonic Anhydrase Inhibitors on Kidney Function:
Carbonic anhydrase inhibitors ultimately cause increased bicarbonate excretion. The urine becomes alkaline, while the blood becomes acidic. Additionally, increased sodium in the filtrate prevents water reabsorption, effectively decreasing plasma volume.
Loop Diuretics (Iris)
- Normal Molecular Mechanism of the Transporter Affected by Loop Diuretics:
The Na+, K+, 2Cl- symporter, a carrier-mediated process, is the major reabsorptive mechanism in the thick ascending limb (TAL). All four ions are transported by secondary active transport into the TAL epithelial cells, at their apical surface, using the energy derived from the Na+/K+-ATPase co-transporter, also a carrier mediated mechanism. (RFUMS, 2006)
- Mechanism of Action of Loop Diuretics:
Loop diuretics act on the Na-K-2Cl symporter in the thick ascending limb of the loop of Henle to inhibit sodium and chloride reabsorption. Because magnesium and calcium reabsorption in the thick ascending limb is dependent on sodium and chloride concentrations, loop diuretics also inhibit their reabsorption. By disrupting the reabsorption of these ions, loop diuretics prevent the urine from becoming dilute and disrupt the generation of a hypertonic renal medulla. Without such a concentrated medulla, water has less of an osmotic driving force to leave the collecting duct system, ultimately resulting in increased urine production. This diuresis leaves less water to be reabsorbed into the blood, resulting in a decrease in blood volume. (Rossi, 2004)
 Source: http://www.clinic-clinic.com/images/phrmclgy/drtcs1.gif
Source: http://www.clinic-clinic.com/images/phrmclgy/drtcs1.gif
- Overall Effect of Loop Diuretics on Kidney Function:
Loop diuretics cause vasodilation of the veins and of the kidney's blood vessels, mechanically causing a decrease in blood pressure. The collective effects of decreased blood volume and vasodilation decrease blood pressure and ameliorate edema. (Thomas, 2000)
Thiazide Diuretics (Kimberly)
- Normal Molecular Mechanism of the Transporter Affected by Thiazide Diuretics:
Thiazide diuretics inhibit the Na-Cl symporter (NCC). This is a channel present on the luminal side of the distal convoluted tubule of the nephron and functions via secondary active transport. Sodium enters the cell down it concentration gradient (“downhill”), while chlorine goes up its electrical gradient (inside of the cell is negative). Chlorine is able to travel “uphill” without direct usage of energy because it uses the energy that sodium dissipates when it goes down its concentration gradient. Once these two ions enter the cell, the sodium is shuttled across the basolateral side of the cell via Na/K ATPase (primary active transport) and chlorine travels across a chlorine channel (facilitated diffusion). (RFUMS, 2006)
- Mechanism of Action of Thiazide Diuretics:
Individuals that suffer from high blood pressure are typically given thiazide diuretics. It is believed that thiazide inhibits the Na-Cl symporter by binding to the Cl- site of the transporter. This shuts down the pump and leads to excretion of sodium and chloride. By inhibiting these solutes to be reabsorbed into the plasma, they will cause the urine to have a greater concentration (increased amount of osmotically active solutes) and this will give water the gradient to remain in the filtrate. Also water will not be reabsorbed in the collecting tubule because the plasma osmolality will be reduced, so it will need to leave the plasma because the extracellular fluid osmolality will be low.
 Source: http://www.mc.uky.edu/pharmacology/instruction/pha824dr/PHA824dr.html
Source: http://www.mc.uky.edu/pharmacology/instruction/pha824dr/PHA824dr.html
- Overall Effect of Thiazide Diuretics on Kidney Function:
Thiazide diuretics are successful at reducing blood pressure because they reduce the plasma volume. It is possible that thiazide diuretics also act to relax the smooth muscle of blood vessels to reduce the resistance to blood flow. Patients that take these medications will tend to have a greater frequency of urination accompanied by increased solute and water loss.
Conditions or Diseases for Which Diuretics are Prescribed (Amanpreet)
Diuretic
A diuretic is essentially an agent that removes water from the body by promoting urine formation and the loss of salt (Sodium)
Uses for diuretics
Since diuretics increase the rate of urine flow. These agents are mainly used in the management of edema and hypertension. However there are several classes of diuretic drugs (Osmotic diuretics, Carbonic anhydrase inhibitors, Loop diuretics and Thiazide) and because of their mechanism of action some are beneficial in control of other pathologies and symptoms. E.g. Some diuretics, such as acetazolamide, help to make the urine more alkaline and are helpful in increasing excretion of substances such as aspirin in cases of overdose or poisoning
Diuretics can be prescribed for the prevention, treatment or improvement of symptoms in a variety of pathophysiologic conditions, such as
- High blood pressure
- Congestive heart failure
- Edema
- Glaucoma
- Polycystic ovary syndrome.
- Certain kidney disorders, such as kidney stones
- Diabetes insipidus
Following are some examples and conditions for which diuretics are considered beneficial
Glaucoma
Carbonic anhydrase inhibitors are used to reduce intraocular pressure in the treatment of glaucoma. These agents inhibit intraocular carbonic anhydrase and thus the formation of aqueous humor.
Congestive heart failure
Heart failure leads to activation of the renin-angiotensin-aldosterone system, which causes increased sodium and water retention by the kidneys. This in turn increases blood volume and contributes to the elevated venous pressures associated with heart failure, which can lead to pulmonary and systemic edema. The primary use for diuretics in heart failure is to reduce pulmonary and/or systemic congestion and edema, and associated clinical symptoms (e.g., shortness of breath - dyspnea).
Pulmonary and systemic edema
Cirrhosis
Renal Insufficiency
Nephrotic syndrome
Diuretics alleviate the symptoms of these diseases by causing sodium and water loss through the urine. Capillary hydrostatic pressure and therefore capillary fluid filtration is strongly influenced by venous pressure .Therefore, diuretics, by reducing blood volume and venous pressure, lower capillary hydrostatic pressure, which reduces net capillary fluid filtration and tissue edema.
Diabetes insipidus
Thiazide diuretics have been known to be beneficial in controlling diabetes insipidus. Although it seems paradoxical to treat polyuria with a diuretic, a net decrease of urine flow occurs with lowering of urine volumes to normal or only slightly elevated values.
Hypercalcemia
Loop diuretics are used to treat hypertension. But the increase in Ca2+ excretion caused by these agents makes them useful in the treatment of hypercalcemia.
Group members
- Iris Corbin
- Soleil Leilabadi
- Christine Mata
- Amanpreet Sherwal
- Sinh Tran
- Kimberly Zamor
Sources
- Rossi S (Ed.) (2004). Australian Medicines Handbook 2004. Adelaide: Australian Medicines Handbook. ISBN 0-9578521-4-2
- Thomas, MC (2000). Diuretics, ACE inhibitors and NSAIDs -- the triple whammy. Med J Aust 172, 184–185. PMID 10772593
- RFUMS Renal Physiology Lectures, Winter Quarter 2006-2007
- STAT!Ref. http://online.statref.com/Document/Document.aspx?DocId=264&FxId=75&Scroll=1&Index=0&SessionId=82BFF1LYFJTGYVXJ
- "Diuretics." Drug Digest. June-July 2006. Express Scripts. 17 Nov. 2006 <http://www.drugdigest.org/DD/Comparison/NewComparison/0,10621,33-17,00.html#>.
- "Pharmacology of Diuretic Drugs." 17 Nov. 2006 <http://www.pharmacology.med.umn.edu/LEE-PHCL5103/04DiureticNotes.pdf>.
- Costanzo, Linda S. Board Review Series Physiology 3rd Edition. Lippincott Williams & Wilkins. 2004.
Comments (0)
You don't have permission to comment on this page.